Healthcare resource allocation and patient choice: evidence from rural China | International Journal for Equity in Health

Benchmark regression results
The impact of optimizing the allocation of healthcare resources in county level hospitals on patients’ choice of healthcare
Table 2 in the first column presents the impact of improving the comprehensive capabilities of county-level hospitals on patients’ healthcare choices. The regression results show that, compared to non-pilot counties, patients in pilot counties significantly reduced their probability of seeking healthcare outside the county. This implies that, following improvements in rural healthcare resources, residents have gained more confidence in the availability and quality of healthcare services within their counties. As a result, more residents have chosen to seek healthcare within their counties. However, as indicated by the descriptive statistics, although this reform has increased the rate of residents seeking healthcare within their counties, there is still room for improvement in achieving the goal of “90% of residents seeking healthcare within the county” in various districts and counties of this city. The reasons for this may include the improvement in transportation convenience and policies such as direct reimbursement for inter-city medical expenses, which facilitates cross-district access for patients. Therefore, continuous efforts are needed in the future to further enhance the layout of high-quality healthcare resources in rural areas, improve residents’ access to high-quality healthcare, and encourage patients to return to their counties.
The impact of enhancing the comprehensive capacity of county-level hospitals on patients’ healthcare burden
Table 2, column (2), demonstrates the influence of enhancing the comprehensive capacity of county-level hospitals on the average inpatient expenses per patient. The regression results reveal that, compared to non-pilot counties, patients with potential demand for seeking healthcare outside their county experienced a significant reduction of 6.3% in their average inpatient expenses. This indicating that the enhancement of county-level hospital capacity significantly reduces the burden of inpatient expenses for patients. One possible explanation is that patients seeking healthcare services outside their county often opt for hospitals in urban areas, where medical equipment is better and healthcare resources are more abundant compared to county-level hospitals. This results in a heavier financial burden for patients. However, with the improved treatment capabilities of county-level hospitals, patients can effectively alleviate their financial burden by receiving medical care within their county. Furthermore, the study finds that inpatient expenses for patients increase significantly with age, aligning with existing literature. This could be attributed to older individuals having poorer physical health, leading to a higher utilization of healthcare resources compared to younger age groups.
The impact of enhancing the comprehensive capacity of county-level hospitals on healthcare quality
The enhancement of county-level hospital comprehensive capacity aims to promote the allocation of high-quality healthcare resources to rural areas through hospital development, thereby providing high-quality medical services to residents within the county. Therefore, the assessment of healthcare quality is a crucial factor in evaluating the effectiveness of healthcare reform. To eliminate the influence of planned hospitalization behaviors, this study excluded patients with a hospitalization interval of less than 2 days between the next admission and the current discharge. To account for the effects of planned hospitalization behaviors, this study also excluded patients who had more than 3 hospitalizations within one year and removed patients with chronic and severe conditions that require regular hospitalization. The standard for measuring healthcare quality was based on non-planned hospitalizations within a specific period. The regression results are shown in Table 3, with columns (1) to (3) representing the two-week readmission rate, one-month readmission rate, and three-month readmission rate, respectively. The results indicate that, following the enhancement of comprehensive capacity in county-level hospitals, the healthcare quality of inpatients has significantly improved, as demonstrated by the reduction in readmission rates within two weeks and one month. However, the three-month readmission rate indicator is not statistically significant, suggesting that the quality of short-term hospital treatment has improved.
Based on the regression results from Tables 2 and 3, it can be observed that improving the allocation of healthcare resources in rural areas not only attracts patients to return for healthcare services within their county, creating an organized healthcare pattern but also enhances the efficiency of healthcare resource utilization. Simultaneously, it allows patients to enjoy better medical services while reducing the financial burden of inpatient expenses. This significantly improves the welfare of patients. Balancing the distribution of healthcare resources between urban and rural areas is an effective method to alleviate the challenges of limited access to medical care and high medical costs faced by rural residents in China.
Parallel trend and robustness tests
Parallel trend test
In this study, the pilot policy of improving the comprehensive capabilities of county-level hospitals is treated as a quasi-natural experiment. The policy effect is estimated using a difference-in-differences (DID) model. To ensure the comparability of the two groups of samples, it is essential to demonstrate that before the pilot, the pilot counties and non-pilot counties had the same trend of changes. We employed an event study approach to perform parallel trends tests, and the model setup is as follows:
$${Y}_{ijt}={\alpha }_{0}+{\sum }_{p=-5}^{6}{\alpha }_{0}{treat}_{ij}*{quarter}_{t}+{\alpha }_{q}{X}_{ijt}+{\mu }_{t}+{\delta }_{i}+{\varepsilon }_{ijt}$$
(3)
Here, \({quarter}_{t}\) represents the quarterly time variable, with the first quarter of 2018 as the base period, to observe how the policy effect changes over time. The remaining variables in Eq. (3) are set the same as in Eq. (1), where \({\beta }_{p}\) is the coefficient of primary interest in this study. Figure 2. is constructed based on the estimated values of \({\beta }_{p}\) and the confidence intervals. Overall, before the policy pilot, pilot counties and non-pilot counties generally exhibit a parallel trend. However, after the policy, the effect gradually becomes apparent. The rate of seeking healthcare outside the county decreases steadily, with a more pronounced decrease in 2020. This indicates that residents’ confidence in local healthcare resources within the county has gradually accumulated. It also suggests that the enhancement of comprehensive capabilities of county-level hospitals has played a significant role in treatment during the epidemic period, meeting the basic medical needs of residents within the county. Regarding the trend in medical quality, it is observed that there is an overall improvement trend in medical quality within the county after the reform.
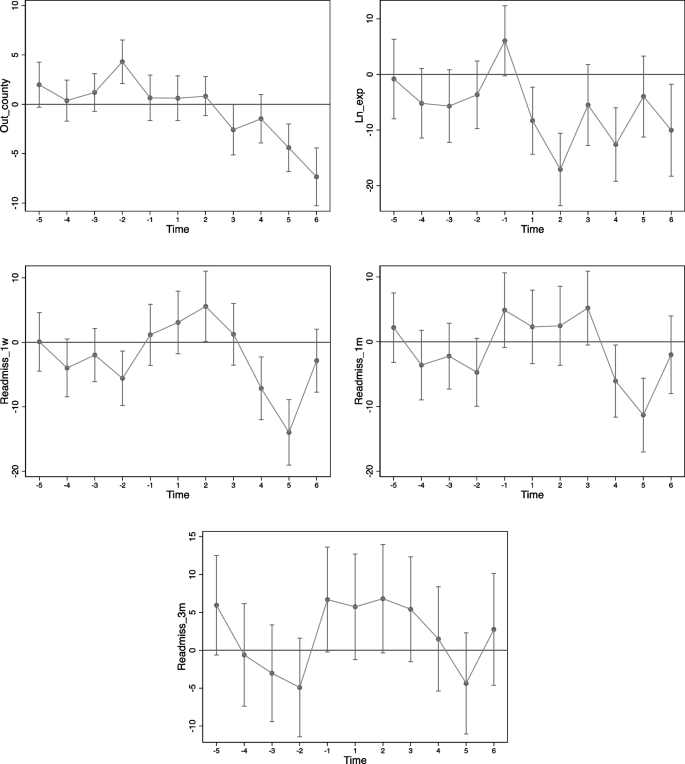
Parallel Trends Test. Note: The horizontal axis represents the number of quarters before and after the announcement of the pilot list, where 1 corresponds to the third quarter of 2019, and −1 corresponds to the second quarter of 2019. The vertical axis represents estimated coefficients and their 95% confidence intervals
Robustness test
First, we need to rule out the impact of the COVID-19 pandemic. In January 2020, there was a global outbreak of COVID-19, which significantly affected residents’ mobility and healthcare-seeking behaviors. During this period, most residents chose not to seek healthcare unless it was necessary, resulting in a sharp decline in outpatient and inpatient visits nationwide. This led to significant structural changes in patients’ characteristics. Therefore, within the analytical framework of this study, the initial impact of the pandemic might have affected the regression results. As shown in Fig. 3, in February 2020, both the polit and non- polit counties experienced a dramatic decrease in the total number of monthly patients seen. However, this trend started to ease in March, with healthcare institutions gradually returning to normal patient volumes. To account for the impact of the pandemic-induced changes in medical demand on the regression results, we conducted robustness tests by excluding data from January to May 2020. The results, as shown in Table 4, remained robust.
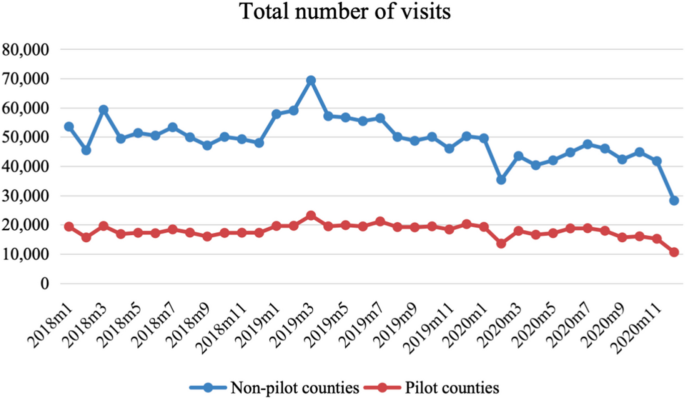
Distribution of Patient Visits
Second, we need to rule out the impact of the poverty reduction policy. During the sample period analyzed in this study, the nation was actively engaged in the critical phase of poverty reduction, with some impoverished areas benefiting from policy support. Health support policies, as a vital component of precision poverty reduction, may have influenced residents’ healthcare needs and the healthcare supply behavior of medical institutions, potentially interfering with the assessment of the policy’s effectiveness in this study. Within this city, six counties were included in the national list of poverty-stricken counties. In September 2018, the city also introduced a health support program aimed at helping poverty-stricken counties in their efforts to reduce poverty. To eliminate the influence of the health poverty support program, this study excluded data from these six poverty-stricken counties and conducted robustness checks. As shown in Table 5, the regression results remained robust.
link








