Determinants of vaccine hesitancy among healthcare workers in an international multicenter study within the EuCARE project
Participants
Overall, 2079 HCWs responded with complete demographic information for regression analysis relating to job, education and place of work for 1907 (Table 1). Only a minimal common dataset was permitted across all the study sites by all the ethics committees. Over a third of respondents (34.9%) were medical doctors.
The distribution of respondents by country was: Lithuania—332, Portugal—409, Poland—445, Brazil—247, and Germany—583. An additional 63 responses were not linked to a specific center. The corresponding response rates were 5.5% for Lithuania, 6.3% for Portugal, 22.3% for Poland, 9.9% for Brazil, and 7.3% for Germany. A core data set for subgroup analysis (n = 1907) was used where individuals had given complete information on their occupation, education level and country of work.
COVID-19 vaccination
The majority, 96.8% (n = 2006) of participants had received COVID-19 vaccination (leaving just 3.2% (n = 67) unvaccinated). Messenger RNA-based vaccines were the dominant vaccine types: in our study, 56.5% of respondents received the Pfizer-BioNTech vaccine, and 17.8% received the Moderna vaccine; 15.3% of respondents received the AstraZeneca vaccine, with smaller percentages for other vaccines. The majority of respondents had received 2, 3 or 4 doses/boosters (23.8% 36.2% and 26.8%, respectively).
While the COVID-19 vaccination rates were high, just over two thirds (67.90% n = 1301) felt that the “COVID-19 vaccination available” to them was safe; 14.7% (n = 282) did not feel the offered vaccines were safe; 14.0% (n = 268) were “not sure” and 3.4% (n = 65) that only some available were safe (Pfizer-BioNTech, Moderna, Coronovac, Spikevac, Johnson and Johnson). Considering further questions around COVID-19 vaccine safety, 45.2% (n = 866) had concerns as to whether they had been adequately tested and 9.6% (n = 183) preferred to obtain their own immunity from getting COVID-19 itself. Specifically, only 55.7% (n = 1068) were “confident about the long-term safety of the COVID-19 vaccine offered” to them with 19.1% (n = 365) indicating lack of confidence, and a similar proportion, 23.4% (n = 448) uncertain with the long-term safety. Individuals were also concerned (27.2%, n = 522) about the immediate/short-term side effects of the COVID-19 vaccine, 10% of those responding (n = 191) believed that the risk of having COVID-19 vaccines was greater than the risk of COVID-19 itself.
When the vaccinated were asked whether they “believed that the COVID-19 vaccines are effective (work well)” 12.7% (n = 243) answered “no” and 17.8% (n = 340) were not sure. The reasons given by the small number of individuals (n = 67) who were not COVID-19 vaccinated mirrored this to some extent: respondents were able to offer multiple reasons for non-vaccination but 14.6% felt it was “a novel vaccine and has been rushed through the development phases” and 11.1% said they “don’t believe it is helpful in preventing COVID-19”. Other major reasons given were “I did not want it” (16.1%); “not offered” (9.1%); “fear of side-effects” (12.6%); “not at great risk from COVID-19” (6.0%); “preferred to take the risk of catching COVID-19” (4.5%); “believe I may be allergic to a component of the vaccine” (4.0%).
Correlates of vaccine hesitancy
Level of education was associated with the degree of vaccination hesitancy. HCWs with Master’s degrees had similar levels of concern regarding the safety and testing of COVID-19 vaccination to those with doctorate-level degrees. However, there was a significantly increased concern in HCWs where the highest qualification was a bachelor’s degree and those with a high school education only (Table 2).
Specific HCWs occupation also had an impact. When compared to medical doctors, allied health professionals and scientists had similar levels of concern but concern (e.g. worry about safety and testing) was significantly higher amongst nurses and administrative staff (Table 2).
Broadly similar rates of concern regarding VH were seen in HCWs in Lithuania, (which received the questionnaire first), Germany and Poland, with lower rates seen in Portugal and Brazil (Table 2).
Sources of vaccine information
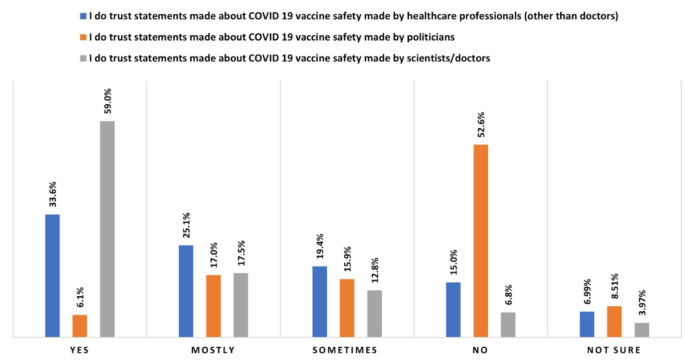
In terms of information sources about COVID-19 vaccination that were most or least trusted (Fig. 1) the majority agreed with the statements “I do trust statements made about COVID-19 vaccine safety made by health professionals or scientists/doctors” (76.5% “trusting” and “mostly” trusting). There was an equally strong negative response to trusting statements “made by politicians” (23.1% “trusting” or “mostly trusting; 52.6% “not” trusting at all). Similar proportions were seen in relation to efficacy (data not shown).

Respondents trust in COVID-19 vaccine safety information from different sources.
Other vaccines
Overall respondents were very supportive of the value of childhood vaccinations and their safety in particular; 80.0% (n = 1500) believed them to be safe with only 5.2% (n = 98) not believing they were safe and 12.3% (n = 231) not sure. An additional 2.5% (n = 47) felt that some childhood vaccines were unnecessary.
We enquired as to whether individuals would like to have an influenza vaccination this year and their influenza vaccination history in previous years. Of those responding only 13.7% (n = 113) said yes, with 67.0% (n = 555) saying no and 14.0% not sure and 5.3% of those asked (n = 44) had already had an influenza vaccination at the time of asking. Only about half of HCWs had had influenza vaccination in previous years (Table 3).
The range of reasons provided by those not taking the influenza vaccine in the past or not planning to accept vaccination this year are presented in Fig. 2; the most common reason being the vaccine was not specifically offered to them (i.e. only a general offer that influenza vaccine was available) and 10.9% did not believe the vaccine to be effective in preventing influenza. A small proportion (1.3%) believed that the vaccine would cause influenza.

Reasons for not taking the influenza vaccine.
Compulsory vaccination
Views on compulsory COVID-19 and influenza vaccination show less consensus for influenza than COVID-19 (Table 4).
Over half of respondents felt that COVID-19 vaccination should be compulsory for all staff working in healthcare settings (unless medically exempt) (54.2%), for all patient-facing healthcare staff (59.0%) and for all medical, nursing and midwifery students (56.7%) (Table 4).
Far fewer supported compulsory influenza vaccination i.e. compulsory for all staff working in healthcare settings (38.0%, for all patient-facing healthcare staff (41.5% and for all medical, nursing and midwifery students (39.7%) (Table 4).
Table 5 examines compulsory vaccination more closely in relation to reference groups (there was complete data for education, occupation, and country for comparison for 1907 participants). There was widespread equanimity for compulsory vaccination of HCWs for COVID-19 and influenza.
We examined whether any HCW subgroups differed significantly in their views on this. Individuals with a high school education or a bachelor’s degree were less likely to support mandatory COVID-19 or influenza vaccination compared to those with a doctorate degree. By professional group, nurses were less supportive of compulsory vaccination.
There was widespread support for mandatory childhood vaccination but administrative staff and academics had a higher probability of concern with the safety of childhood vaccinations.
Compared to Lithuania as a reference country on compulsory vaccination, Brazil was more likely to support compulsion for both COVID-19 and influenza vaccination whilst Germany leant the other way.
Table 6 is colour coded based on the “Three Cs” i.e. Red for Convenience (practical, access issues) (CONV); Blue for Confidence (CONF) and Green for Complacency (COMP).
Within the HCW cohort, we explored whether education level, individual healthcare worker occupation, or country of origin had an impact on the importance of the above factors and whether there were national differences (Table 7). Regarding education, compared to participants with doctoral-level education, those with lower education levels, including high school and bachelor’s degrees, had significantly higher odds of reporting that “Opportunity to ask questions and think about the vaccine before making a decision” and “Information available from official international bodies” were not factors in getting COVID-19 vaccines (AOR > 1). Those holding a bachelor’s degree had significantly higher odds of reporting that “enough information about the safety of the vaccine” was not associated with COVID-19 vaccination whilst “wanting to visit vulnerable family or friends” was more likely to be associated.
Other factors appeared to be similarly reported across education levels. By professional qualifications, nurses and allied health workers showed significantly higher odds of reporting that “Enough information about the safety of the vaccine” and “Information available from official international bodies” were not factors in getting COVID-19 vaccines, compared to doctors. Additionally, scientists and midwives had higher odds of reporting that “Available at my place of work during working hours” was not a factor in getting COVID-19 vaccines, compared to doctors.
Key influencing strategies showed significant geographical disparities. For example, compared to Lithuania, HCWs in Poland, Portugal, and other countries, showing significantly higher odds of reporting that vaccine availability at their place of work was not a factor in getting COVID-19 vaccines. In contrast, individuals in Brazil, Portugal and Germany showed higher odds of reporting that “Opportunity to ask questions and think about the vaccine before making a decision” and “Information available from official international bodies” were significant factors in getting COVID-19 vaccines (AOR < 1).
HCWs in Germany and Portugal, reported that “leaders/management in their organisation having a vaccine” were significant factors in promoting vaccination.
link








